SUMMARY
This is AI generated summarization, which may have errors. For context, always refer to the full article.
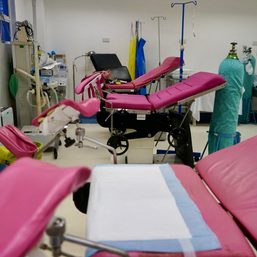
![[OPINION] Will a coronavirus vaccine reach developing countries in time?](https://www.rappler.com/tachyon/r3-assets/612F469A6EA84F6BAE882D2B94A4B421/img/8549AA86C6FA472B873B65191FCCB439/will-a-covid-19-vaccine-reach-developing-countries-in-time.jpg)

In a developing nation, those who can shelter in place co-exist with those who cannot. Not everyone has a home. Not everyone wears masks. People will go about their business at the risk of getting sick, not because they want to violate orders, but because they need to survive.
In our invisible war, the only way to really ensure public health safety is through a vaccine.
Unfortunately, once that vaccine for COVID-19 ships, everyone in the world would want it (except maybe anti-vaxxers who seem to prioritize their beliefs more than science).
Countries, where the laboratories working on a vaccine are located, will get first dibs. Countries with the resources that the Philippines does not have will be first in line. The US, the current epicenter of the pandemic, will likely buy in the truckloads because they have more deaths, with COVID-19 cases there now approaching 2 million out of the total 6 million confirmed cases globally.
This is the grim scenario I foresee as a citizen of a country constantly at the lower end of the global economic spectrum. But in the sphere of public health, the Philippines and other developing nations should matter, despite our seeming irrelevance on the world stage. We have done what we could in sheltering our people and lowering the death toll. We need the COVID-19 vaccine just as much as every country does. (READ: The latest in the global race for a coronavirus vaccine)
The question is, will we have equal access to the vaccine once it is ready to go to market?
How a vaccine is developed
The process of creating a safe vaccine is lengthy, complex, and expensive. It requires at least a billion dollars and around 10 years to deliver a final, licensed vaccine.
This makes vaccine development an investment usually reserved for rich states that can finance vaccine research entities and partner with top vaccine-producing pharmaceutical companies.
Given the mounting global death toll, the race to find a safe and effective COVID-19 vaccine is on. As the new chief economist of the World Bank Carmen Reinhart has said, “If it’s not over on the disease, it’s not over on the balance sheet.” We have to win the war against COVID-19 to get our lives and livelihoods back, and the most effective way to do that is through a vaccine.
Production woes
Additional factories will have to be built, ideally once a vaccine has been approved because the requirements of an inactivated vaccine, for example, are different from that of an RNA vaccine.
Vaccines have to be refrigerated at a storage temperature of at least 5 degrees C, which makes the global shipment of 16 billion doses no mean feat.
We need more than one pharmaceutical company to handle global demand, so the European Union (EU)’s proposal to encourage companies to give up their monopolies on vaccines could help with rapid mass production.
Infectious diseases still cause almost 30% of all deaths worldwide. The demand for their vaccines remains high. How do you manufacture a COVID-19 vaccine while still producing existing vaccines? How do you prevent a shortage in production?
Will the vaccine be equitably distributed? Not likely, but it is still possible. The US Biomedical Advanced Research and Development Authority (BARDA) already said that their focus is on the “whole-of-America approach required to expedite the availability of vaccines.” BARDA has channeled substantial resources for Johnson & Johnson, French drug company Sanofi, and Massachusetts-based Moderna.
This does not bode well for developing countries, but the WHO, having learned its lesson from the inequitable distribution of vaccines for HIV and H1N1, has made information on the development and the deployment of the vaccine to be equally available to all.
Vaccines require syringes, wipes, and medical adhesives to administer. Can countries hoard these materials in the same way that PPEs were embargoed? Yes, especially countries where these products are manufactured. We saw that in the mad scramble for PPEs.
Will the COVID-19 vaccine reach developing nations in time? It could, through the help of organizations such as the Global Alliance for Vaccines and Immunisation (GAVI). As of 2019, there are 58 developing countries that are eligible for vaccine support.
AstraZeneca has also declared that it is partnering with other companies for simultaneous production, which include Serum Institute of India, a major supplier of vaccines to the developing world.
There is also a global call for a “people’s vaccine.” Oxfam, an international non-profit organization, has published an open letter from 140 world leaders and experts “calling on Health Ministers at the World Health Assembly to rally behind a people’s vaccine…produced rapidly at scale and made available for all people, in all countries, free of charge.”
What developing countries can do
The odds are not all stacked against developing countries, especially if there is a designated committee that can already lay the groundwork now for this massive vaccination program in cooperation with other governments.
There is a scene in the movie Contagion about inoculation lotteries, which looked rather organized, but chaos still ensued. The COVID-19 vaccine committee should have the right people in their team that can quell possible anarchy.
Governments should coordinate with the WHO regarding licensing requirements for the local manufacture of vaccines. They can closely track the developments in foreign laboratories that are already at phases 1 and 2 of their clinical trials. Finding a local firm that meets the global standards of an RNA vaccine manufacturer, say, is a long shot, but it is still a shot worth taking.
Developing countries should start preparing for vaccination kits and their contents to avoid having to compete with other countries for supplies. Since most medical supplies are being used now for COVID-19 cases, local pharmaceutical companies may want to ramp up production for vaccine-specific requirements such as wipes and syringes.
While our public health professionals are hard at work fighting this war for us, our ambassadors can start forging partnerships with their counterparts and other stakeholders in the international health community. They can look into procuring vaccines from the nearest first world neighbor where they have friendly relations which could be Singapore or even China which has labs developing a vaccine for Southeast Asian countries. They need to sort out tariffs and bottlenecks in the global supply chain for medical materiel as early as now to reduce unnecessary delays. No one wants another end-run where one country is accused of hijacking a shipment of PPEs already purchased by another country. This can be avoided through peaceful diplomacy.
All government hands in developing countries should be on deck to help make sure that when the vaccine is finally available, we will have access to it. Public officials who work outside of public health can start planning for this now. Living conditions in developing countries are far more desperate than in other countries, and there is a global initiative to help everyone access the vaccine. We just need to make sure we are not overlooked. – Rappler.com
Mai Mislang is a writer, consultant, and musician. She served as Assistant Secretary of Presidential Communications at Malacanang from 2010-2013.
Add a comment
How does this make you feel?

![[In This Economy] Can the PH become an upper-middle income country within this lifetime?](https://www.rappler.com/tachyon/2024/04/tl-ph-upper-income-country-04052024.jpg?resize=257%2C257&crop=295px%2C0px%2C720px%2C720px)


There are no comments yet. Add your comment to start the conversation.