SUMMARY
This is AI generated summarization, which may have errors. For context, always refer to the full article.
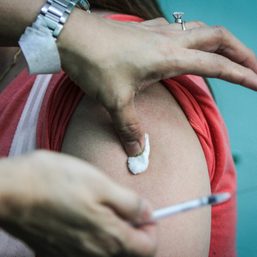
![[OPINION] Vaccinating Persons Deprived of Liberty must be a gov’t priority](https://www.rappler.com/tachyon/2021/09/delta-variant-pdls.jpg)
The Philippines has the most overcrowded correctional system in the world, with an average congestion rate of over 460%. In a few jails, the congestion rate hovers over 2,600%. This level of overcrowding poses immense correctional management challenges, which are now stressed even further with the threat of the spread of COVID-19 amongst the inmates – referred to here as Persons Deprived of Liberty (PDLs). Under such heavily congested conditions, there is a high degree of probability that PDLs will contract COVID-19, and that PDLs are at a greater risk of harm when they get infected.
The relatively recent onset of the Delta variant of the COVID-19 virus is now likely to exasperate the prevalence of infections amongst PDLs in the Philippines. All airborne diseases like COVID-19 can be spread quickly when there is increased contact between PDLs, poor ventilation in cells, and a shorter time spent outdoors due to added lockdown restrictions.
But there are other challenges.
A lack of adequate space to isolate or quarantine infected PDLs is also problematic. There also continues to be risks associated with inadequate sanitation and hygiene provisions, and the added restrictions also greatly exacerbates the physical and mental well-being of PDLs. Such restriction can potentially lead to added tensions, facility disturbances, and PDL violence, as we are starting to witness now.
The added constraints also translate to health services being inadequate and failing to reach vulnerable PDL groups. Almost one-third of people entering correctional and detention facilities have a mental health or chronic medical condition like asthma, cancer, cardiovascular disease, or diabetes, or live with disability. Elderly PDLs, those with mental health conditions, and those with TB, diabetes, and other significant health issues, are particularly vulnerable to the Delta variant.
The challenges from the lockdown restrictions don’t end there. As legal visits have been suspended, PDLs face even longer time in jail while undergoing trial. Most hearings are now conducted online – a great innovation introduced by the Supreme Court – but still many facilities lack structural support, like computers and internet connections. This has led to numerous hearing postponements and the re-setting of trials to indefinite dates.
The jail and prison officials (the Bureau of Jail Management and Penology [BJMP] and the Bureau of Corrections [BuCor], respectively) have sacrificed much to keep the PDLs free from COVID-19 infection.
Staff have stayed in jail and prisons for prolonged periods of time (28 days straight) and sacrificed spending time with their families in order to minimize their exposure, and the PDLs under their care, to the virus. They also created novel protocols on infection, prevention, and control of COVID-19, trained their personnel to follow the protocols, and implemented these protocols innovatively despite the lack of medical resources, equipment, and personnel. Many jail wardens and prison superintendents developed strong ties with local government units, local hospitals, and non-governmental organizations, in order to address their own resource shortfalls. In cooperation with PDL groups and gangs, they also innovatively transformed cells into COVID-19 quarantine areas and trained PDLs with medical skills to assist as health facilitators.
Yet, two years into the pandemic, all these innovative approaches are under strain and becoming no longer sustainable. The lack of visitations, in particular, have slowly impacted on the mental health of the PDLs, and tensions have begun to boil. A week ago, PDLs from a jail in Metro Manila held a jail officer hostage, demanding their release. This led to the death of two PDLs and a jail personnel. In return, the BJMP instituted more strict measures to prevent a reoccurrence of the hostage taking event.
Balancing the security of correctional facilities with measures to stop the spread of COVOID-19 at the source will always be challenging. Current measures to reduce transmission where possible – including frequent hand washing, wearing masks, physical distancing, good ventilation, and avoiding overcrowding – will continue to impede the amount of viral transmission and therefore also reduce opportunities for the virus to further mutate. But measures to reduce overcrowding to allow these practical measures to work effectively will be impossible in the short term, as security also needs to be upheld.
The long-term solution will be to prioritize the vaccination of all PDLs and staff. Given the overcrowding, they are the group most susceptible to a potential Delta outbreak. Prioritizing PDLs to get vaccinated is a sound public health strategy, as many of them will eventually be released into the community. Vaccinating PDLs is also consistent with the international standards on the humane treatment of prisoners. Vaccines will be a critical tool, therefore, in the battle against COVID-19 in the Philippines’ correctional system, and there are clear public health and lifesaving benefits to using vaccines at the government’s disposal.
The risk of contracting COVID-19 and dying from it are much higher inside prisons and jails compared than outside. The correctional agencies (BJMP and BuCor) must not put off getting PDLs vaccinated. The jail and prison officers have gallantly sacrificed themselves and developed practical on-the-ground measures to minimize infections in their facilities up until now. It’s now the government’s turn to step in and ease the burden of BJMP and BuCor by doing all it can to ensure PDLs are vaccinated in the Philippines’ correctional system. – Rappler.com
Raymund E. Narag, PhD is Assistant Professor at the Department of Criminology and Criminal Justice at Southern Illinois University Carbondale.
Clarke R. Jones, PhD is a Senior Research Fellow at the College of Health and Medicine at Australian National University.
Add a comment
How does this make you feel?
![[OPINYON] Pangangalaga sa mga Persons Deprived of Liberty](https://www.rappler.com/tachyon/2020/12/ispeak-pdl-1280.jpg?fit=449%2C449)

![[Time Trowel] Evolution and the sneakiness of COVID](https://www.rappler.com/tachyon/2024/02/tl-evolution-covid.jpg?resize=257%2C257&crop=455px%2C0px%2C1080px%2C1080px)



![[OPINION] ‘Some people need killing’](https://www.rappler.com/tachyon/2024/04/tl-some-people-need-killing-04172024.jpg?resize=257%2C257&crop_strategy=attention)
![[Judgment Call] Resisting mob mentality for warrantless arrests](https://www.rappler.com/tachyon/2024/04/judgement-call-mob-mentality.jpg?resize=257%2C257&crop=352px%2C0px%2C720px%2C720px)



There are no comments yet. Add your comment to start the conversation.