SUMMARY
This is AI generated summarization, which may have errors. For context, always refer to the full article.
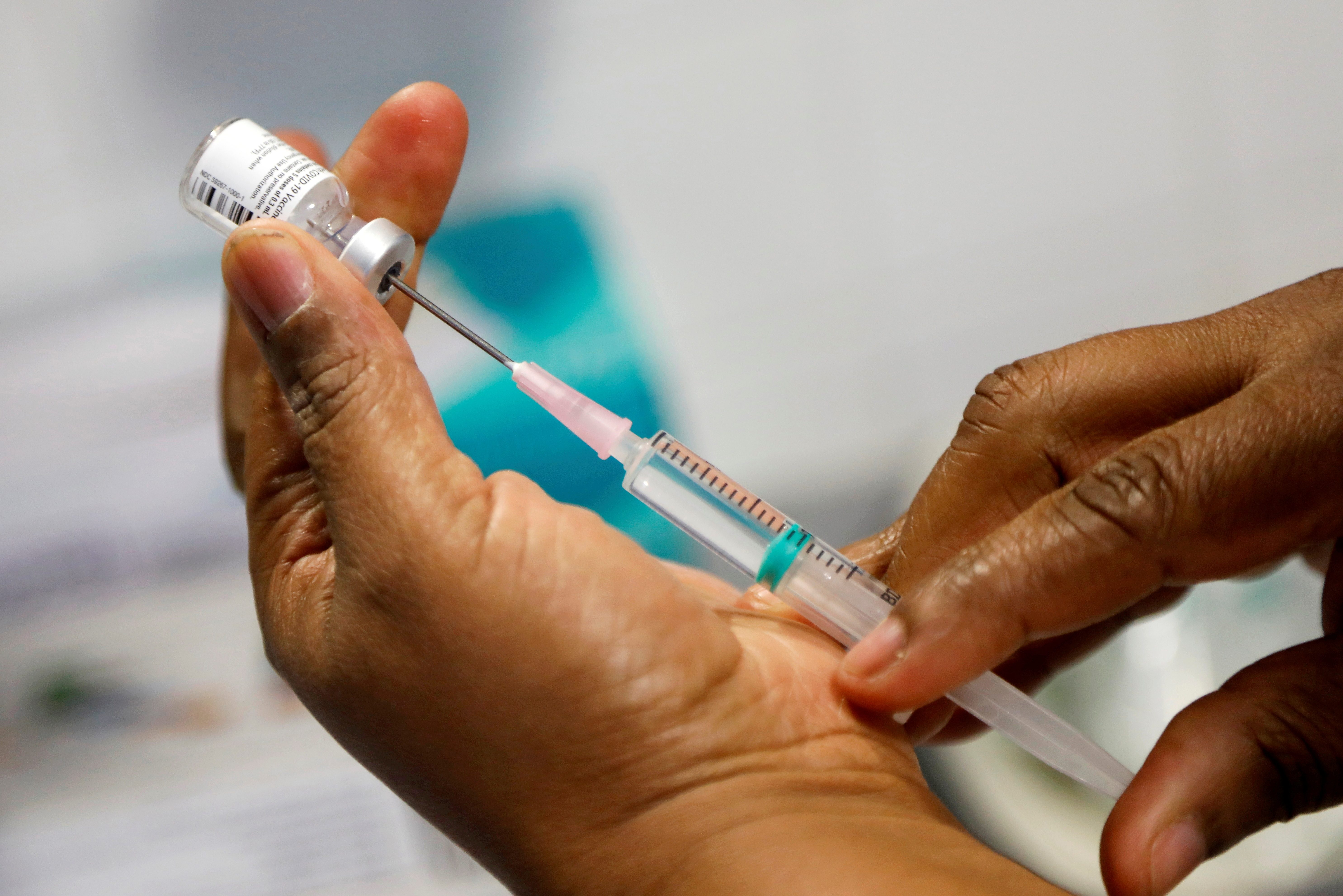
Owing to the urgency of a pandemic, President Rodrigo Duterte signed an executive order (EO) granting the Food and Drug Administration (FDA) the authority to issue emergency use approvals for vaccines and medicines that would combat the new coronavirus.
The EUA is a first-of-its kind in the Philippines, clearing the way for products it covered to be used by the public even while these are still in the development phase.
Under this process, FDA Director General Enrique Domingo said regulators make use of a “risk-based evaluation” where experts weigh a vaccine’s risks against its expected benefits to assess both its quality and the safety of people expected to receive it.
The granting of EUAs is intended to ensure timely access to medicines and vaccines by cutting down the approval processes that normally take 6 months to just about a month.
Here’s what you need to know about how the FDA plans to issue emergency authorizations.
What is it?
While an EUA will allow vaccines and medicines to be used by the public, it is not equivalent to a certificate of product registration or authorization to market the product.
Since COVID-19 vaccines are still considered to be in the development phase, health experts have emphasized that stricter conditions on its use and monitoring are needed. A significant part of granting an EUA to a vaccine is tight surveillance of patients post-immunization, the FDA added.
“Kailangan very strict ang ating monitoring kasi lahat po ng babakunahan talagang kailangan babantayan po natin para maghanap po tayo ng mga adverse events,” Domingo said.
(Our monitoring needs to be very strict because everyone who will get vaccinated will really need to be watched so we can look out for any adverse events.)
Similar to monitoring done in countries like the United States and United Kingdom, close surveillance allows health professionals to respond to adverse events and ensure people remain safe.

Why did Duterte need to sign a special order for it?
Under the FDA Act of 2009, there is no provision that allows the FDA to grant authority to use a drug or vaccine that is still being developed even if a public health emergency calls for it.
Without a special order from the President, a vaccine can only be administered to the public through its inclusion in Phase 3 clinical trials as an “investigational drug” or through a Compassionate Special Permit (CSP). A CSP is given to patients who are sick with illnesses that have no known cure or treatment.
“So, in this case we have a national health emergency in the Philippines and we have a pandemic worldwide. So we really need emergency use for drugs to tame COVID-19 quickly,” Domingo said.
What are the conditions?
The FDA’s Circular No. 2020-036 outlined that an EUA can be issued and will remain valid only when all 3 of the following circumstances are applicable:
- “Based on the totality of evidence including data from adequate and well-known controlled trials, it is reasonable to believe that the drug or vaccine may be effective to prevent, diagnose or treat COVID-19.”
- “The known and potential benefits of the drug or vaccine…outweigh the known and potential risks, if any.”
- There is no adequate, approved, and available alternative to the drug or vaccine.
Aside from the conditions listed, the FDA said an EUA will remain valid only while there remains a public health emergency due to the coronavirus, or until a full market authorization is issued.
If the public health emergency status is lifted or a COVID-19 drug or vaccine is already fully registered with the FDA, its EUA will be valid for one year – from the date it is registered or from when the emergency ends – to exhaust remaining stock of the product.
Domingo said that in the next few years when vaccines are fully registered and granted marketing authorizations, “then the EUAs will cease to exist.”
Who can apply?
Both the pharmaceutical industry and Philippine government can file an application for an EUA with the FDA.
For those in the pharmaceutical industry, this includes vaccine development companies, manufacturers, or importers and distributors of vaccines in the country.
The FDA said national procurers or the Department of Health (DOH), which has the mandate to implement public health programs, can also apply for an EUA.
Domingo said the agency will only accept applications for vaccines or drugs that have been granted an EUA by similar national regulatory authorities in their respective countries or mature and established FDAs such as those listed below:
- United States Food and Drug Administration
- Therapeutic Goods Administration (Australia)
- European Medicines Agency
- Health Sciences Authority (Singapore)
- Pharmaceutical and Medical Device Agency (Japan)
- Ministry of Food and Drug Safety (South Korea)
- Medicines and Healthcare Products Regulatory Agency (United Kingdom)
- Swiss Agency for Therapeutic Products (Switzerland)
- Health Canada
“Hindi pupuwedeng sa Pilipinas unang kukuha ng EUA (They cannot get an EUA from the Philippines first),” Domingo said.
The FDA said this was necessary as evaluations will be facilitated through “reliance and recognition pathways.” These help to speed up approval by allowing the FDA to refer to assessments made by its counterparts listed above when deciding whether a product may be used in the Philippines.
Domingo noted that approval from another regulatory body abroad would not serve as an “automatic stamp” for similar approval in the Philippines. Regulatory officials and health experts here will still need to assess a vaccine’s scientific data to determine implications on its safety and efficacy for Filipinos.
Other than these, vaccines pre-qualified by the World Health Organization may also be considered for recognition. Here, the FDA accepts the decision of the WHO since its requirements would be sufficient to meet those of the Philippines as well.
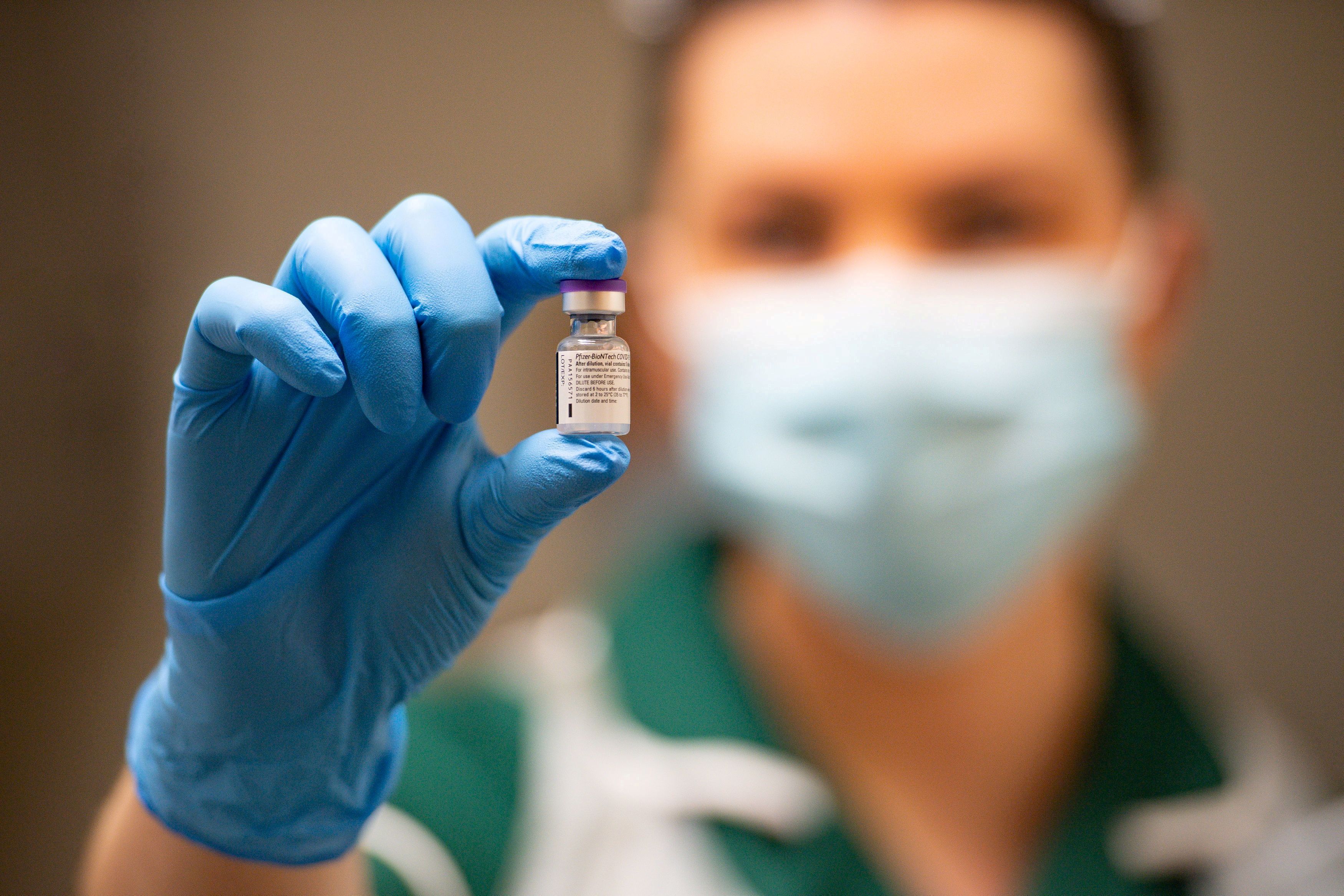
Who has applied so far?
Domingo said only Pfizer has applied for an EUA for its vaccine so far. The company submitted its application late afternoon of December 23 and it is currently being evaluated by the FDA.
A decision may be made mid to late January, he added.
What are the requirements?
Groups that apply for an EUA must ensure that the following requirements to support their application are given to the FDA:

The FDA said it may also require additional documents if these are necessary for review.
Apart from these, companies and manufactures would need to commit to completing clinical trials and development of their vaccine. “They cannot stop after one or two years, they need to complete development and full registration of the product,” Domingo said in Filipino.
What’s the process?
After requirements are submitted, the FDA Director General’s office will determine the completeness of applications. Following this, documents will be referred to the agency’s Center for Drug Regulation and Research and a separate ad hoc panel of experts formed specifically for the review of vaccines seeking EUAs.
Assessment by these two groups will be done simultaneously with the FDA’s CDRR reviewing the technical aspects or quality of the vaccine, and the expert panel reviewing its safety and efficacy.
The panel – whose membership will remain “strictly confidential” – will be composed of at least 3 experts on drugs and vaccine development, immunology, infectious disease pharmacology, and public health toxicology.
Under its review, the panel will determine if based on evidence, it is “reasonable to believe” that a drug or vaccine may be effective in preventing, diagnosing, and treating COVID-19. The group will also weigh the known and potential benefits of a vaccine or drug with its risks, if any.
Once reviews are completed, the expert panel will be responsible for drawing up recommendations to the director general.
Only the FDA director general can approve applications for EUAs.
Drugs and vaccines given an EUA may be subject to special conditions for use, like restrictions on advertising and promotion, reportorial requirements on the safety and effectiveness of products, and strict monitoring to look out for adverse events.
Can the FDA reject applications?
Yes it can, if an application does not satisfy all 3 conditions for the issuance of an EUA. The FDA can also reject it if the drug or vaccine fails to demonstrate safety, efficacy, and quality.
Applications may be denied if there is a failure to disclose relevant information or settle “unresolved” issues on quality, safety, and effectiveness.
Apart from these, the FDA can also reject applications if the product’s label is false and misleading.
Decisions to reject applications will be “final and irrevocable,” the FDA said, though applicants may re-apply if issues raised have been addressed.
Can an EUA be revoked?
The FDA can revoke an EUA if there are violations in “pharmacovigilance obligations” and post-authorization commitments. Domingo said emergency approval can likewise be stopped if “some risks or some unknown adverse events” crop up.
What are the safeguards?
Once approval is granted, EUA holders must observe “ultimate responsibility” for monitoring the safety of their products, the FDA said. This includes proper storage and supply control until delivery.
The FDA and DOH will also conduct post-authorization monitoring to track the deployment of vaccines and drugs, whether cold storage requirements are being followed, and possible side effects and reactions.
EUA holders will need to comply with risk management plans that include sharing information on evolving risks of the product and ongoing, new, or additional studies, among others.
Companies must also report any changes in labeling and manufacturing to the FDA.
In addition to these, the FDA may also coordinate with their counterparts in different countries using the same drugs or vaccines to observe wider monitoring of possible side effects that should be checked in the Philippines. – Rappler.com
Add a comment
How does this make you feel?

![[Rappler’s Best] US does propaganda? Of course.](https://www.rappler.com/tachyon/2024/06/US-does-propaganda-Of-course-june-17-2024.jpg?resize=257%2C257&crop=236px%2C0px%2C720px%2C720px)


There are no comments yet. Add your comment to start the conversation.