SUMMARY
This is AI generated summarization, which may have errors. For context, always refer to the full article.
AT A GLANCE
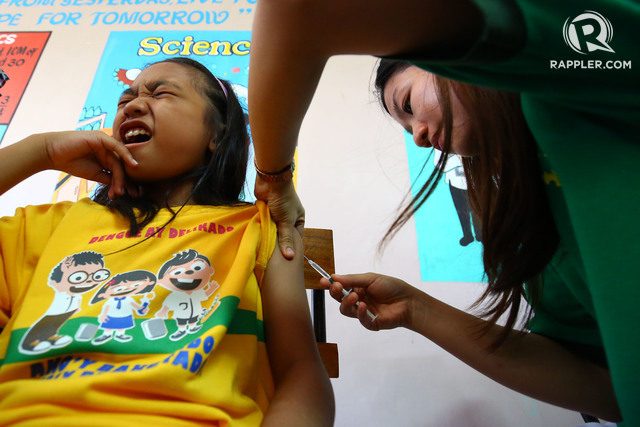
- The Department of Health has spent much of 2018 trying to recover from its Dengvaxia dengue vaccine controversy
- Dengvaxia has contributed to low immunization rates with only 6 out of 10 children receving scheduled vaccines as of November 2018
- Accumulation of unvaccinated children has lead to several measles outbreaks with supplemental immunization activities seeing dismal results
Part 1 of 2
MANILA, Philippines – The Department of Health (DOH) was in the middle of a celebration: its members were welcoming back their former leader, Francisco Duque III, with the good news that the Philippines had finally eliminated maternal and neonatal tetanus.
It was an achievement 11 years in the making as the department first set its sights on it the last time Duque was in office.
But the festivities would not last. Right after the group snapped a celebratory photo, National Immunization Program (NIP) Manager Wilda Silva received a phone call.
“We have a problem,” was the message Silva told Rappler she got November 29, 2017. Today, that problem is one the DOH still finds itself recovering from a year later.
French pharmaceutical giant Sanofi Pasteur made the announcement that night, that its Dengvaxia dengue vaccine poses more risks to people who have not been infected by the virus before immunization.
What the company was essentially saying was that in rare cases, the treatment can actually backfire: Dengvaxia was not guaranteed to prevent dengue after all, and those who never had dengue were at risk of developing a more severe form if infected them later on.
What came next was a flurry of headlines that screamed children died due to the vaccine and health experts warning of its adverse impact on public health programs. They made appeals to be wary of “wild claims,” and urged the public to continue receiving vaccinations as a life-saving measure.
Meanwhile, former president Benigno Aquino III appeared in congressional inquiries where lawmakers and government officials scrambled to pin down who to blame for the mess.
Never mind that it was the first promising vaccine for dengue – a mosquito-borne disease which affects 390 million per year worldwide. Or that it’s one about half of the world’s population is at risk of contracting, according to the World Health Organization (WHO).
The damage was done and trust in experts eroded.
More importantly, there were now over 830,000 students to take care of after the government decided to launch in 2016, its mass school-based immunization program for public school children under then-health secretary Janette Garin. (TIMELINE: Dengue immunization program for public school students)
“Not only did people lose confidence in the immunization program, there was a general loss of confidence in the department…. Right after the announcement… we were down to a 60% approval rating, which was unheard of in the Department of Health,” its Undersecretary Enrique Domingo told Rappler in an interview.

Expecting the worst
Lower trust ratings in the DOH translated to what doctors feared the most: low immunization coverage and outbreaks left and right.
A year after the controversy, Domingo said immunization rates have yet to recover. Only 60% of children were receiving their scheduled vaccines, he said.
It’s the same figure that the DOH saw in April this year and one which they’ll likely end the year with as it remains unchanged. The DOH’s annual vaccination target rate is pegged at about 85% to 90%.
Compared to the previous year, this would be a 10% drop, as the DOH saw 70% of children receive their basic vaccination, according to the 2017 National Demographic Health Survey. Data for 2018 is not yet available as of posting.
Silva said coverage rates for fully immunized children were also at a low 69% from the previous year’s results ranging from 79% to 90%. For children to be considered fully immunized, they should receive the following vaccines:
- Bacillus Calmette–Guérin (BCG) for tuberculosis
- Oral Polio Vaccine (OPV)
- Diphtheria, Tetanus, Pertussis, Hepatitis B, and Haemophilus influenzae Type B (DPT-HepB-HIB)
- Measles, Mumps, Rubella (MMR)
“It’s really like birthing pains all over again. Not just Dengvaxia [was discredited] but the entire [list of] vaccines that we’re using. Even in the budget hearing in Congress, they were starting to question our Tetanus Toxoid vaccine, [saying] that it’s abortifacient,” Silva said.
She added health officials ended up having to submit documents they first gave to lawmakers over a decade ago.
During a media forum in September, Silva also said accounts from health workers showed that parents were still scared of availing of the government’s free vaccines. (READ: Mother of child who got Dengvaxia asks Garin, ‘Nakakatulog pa ba kayo?’)
“They went door-to-door for measles vaccination. And when [health] workers went to homes, mothers would hide their children,” Silva said in Filipino.
Domingo likewise told reporters then that in Metro Manila, health workers would spend up to 30 minutes to convince parents to have their children vaccinated. Even then, consent wasn’t always a guarantee.
“But how do you talk to a million parents? We have to find that way to do it, to turn it into a personalized [thing],” Domingo said, noting it often would help to calm parents down.
“Pero siyempre pag-uwi nila, nandoon pa rin ‘yung [fear] (But when you leave them, there will always be that [fear]). At the back of your mind there will always be that doubt…. It’s that lingering doubt when you have a child vaccinated and you hear that it might cause death,” he added.
Behind the DOH’s low immunization rate was also the fact that its school-based immunization program was hit hard. Whereas Brazil administered the dengue vaccine to those at least 15 years old, the Philippines was the only country that carried out mass vaccination programs on elementary school children.
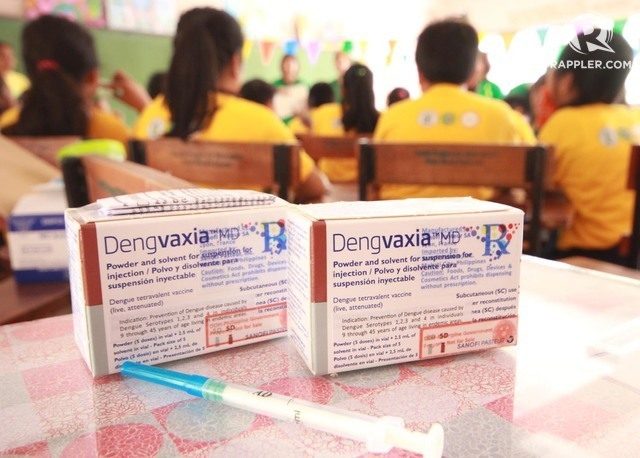
Focus group discussions with health workers, community members, and local leaders done by the DOH revealed this much, since this was the platform used to administer the risky dengue vaccine.
For the DOH, this was a problem. It’s through the regular school-based program that vaccines for diseases like measles, rubella, tetanus, diphtheria, and cervical cancer are often given to elementary students. This, because for many of these vaccines, the age of these students are when treatment is most effective.
Apart from this, another low was seen in the drastic drop in the human papilloma vaccines (HPV) for the cervical cancer program. From 77% of female students covered for its first dose – given before the Dengvaxia scare – only 8% availed of the second dose afterwards, Silva said.
“It’s a very good vaccine, very expensive, but very good vaccine for the protection of women against cervical cancer. But then because of misinformation and fear brought about by the dengue vaccination and the loss of trust in the entire immunization program, this happened,” Silva added.

Containing outbreaks
But perhaps the most adverse effects were seen in the measles outbreaks the DOH declared in 2018 in major areas including Negros Oriental, a barangay in Taguig, Zamboanga City, Davao Region, and Davao City.
The outbreaks, Silva said, were a result of a mix of factors such as the low immunization rate in the aftermath of Sanofi’s announcements and also the growing number of unvaccinated children the DOH had accumulated years before.
“The rule of thumb is if your unvaccinated is equal your target to be vaccinated then you are at very high risk of having an outbreak…. You don’t want your unvaccinated to accumulate throughout the years,” she said.
According to Silva, a study of a 3-year trend for vaccination showed its immunization programs weren’t keeping up with the pace of population growth. And so, it saw a growing number of children who had not yet been immunized.
“We were studying the trend and last year I was talking to the managers, I said you are at risk – actually everyone is – in the situation of an impending outbreak unless you do something,” she said.
What became clear, however, was that the efforts done by the DOH to mitigate risks would be overshadowed by the panic and concern felt all over the country from Dengvaxia.
So even when the health department launched its supplemental immunization program for measles called “Ligtas Tigdas” in April 2018, results were a mixed bag.
While 85% or 9 out of 10 children received the measles vaccine in Mindanao, the same could be said for only 36% or about 4 in 10 children in the National Capital Region.
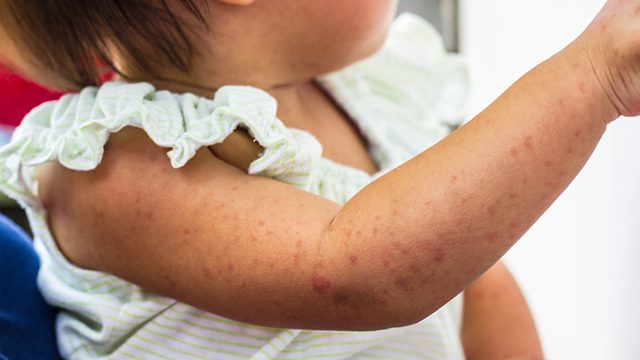
Months later, the DOH isn’t in the clear yet.
This week alone, it announced it was monitoring another suspected measles outbreak in Malapatan town in Saranganil, after 18 children in remote communities died, possibly due to the disease.
Looking at the entire country, data from the DOH’s Epidemiology Bureau showed that measles cases were up by 367%. From January 1 to November 10 this year, 17,298 cases were recorded, whereas the same period last year saw about 3,706 recorded cases.
This, as neighboring countries like Singapore eliminated measles, while Australia, Brunei Darussalam, and Macau eliminated rubella as public health problems, according to the WHO.
“Measles control will not be achieved on time. Measles and rubella elimination targets are off-track…outbreaks continue and progress has slowed,” Silva lamented. – with reports from Vernise L. Tantuco/Rappler.com
(PART 2: Post Dengvaxia controversy: Paving the way forward for vaccines, health care)
Add a comment
How does this make you feel?








![[Rappler’s Best] Patricia Evangelista](https://www.rappler.com/tachyon/2024/04/unnamed-9-1.jpg?resize=257%2C257&crop=486px%2C0px%2C1333px%2C1333px)


![[OPINION] Where are the community libraries 30 years after we passed the law?](https://www.rappler.com/tachyon/2024/06/tl-barangay-public-libraries.jpg?resize=257%2C257&crop=195px%2C0px%2C720px%2C720px)



There are no comments yet. Add your comment to start the conversation.